The digital transformation of healthcare has revolutionized risk assessment and preventive medicine through sophisticated interactive calculators and health assessment tools that provide personalized, evidence-based risk stratification and clinical decision support.
This comprehensive analysis examines the leading interactive risk calculators and health assessment tools across multiple medical domains, evaluating their accuracy, usability, innovation, and clinical impact. Through systematic evaluation of 20 premier tools spanning cardiovascular risk assessment, cancer screening, mental health evaluation, diabetes prediction, and surgical risk calculation, this report identifies the most effective digital resources for both healthcare providers and patients seeking evidence-based health risk assessment and preventive care guidance.
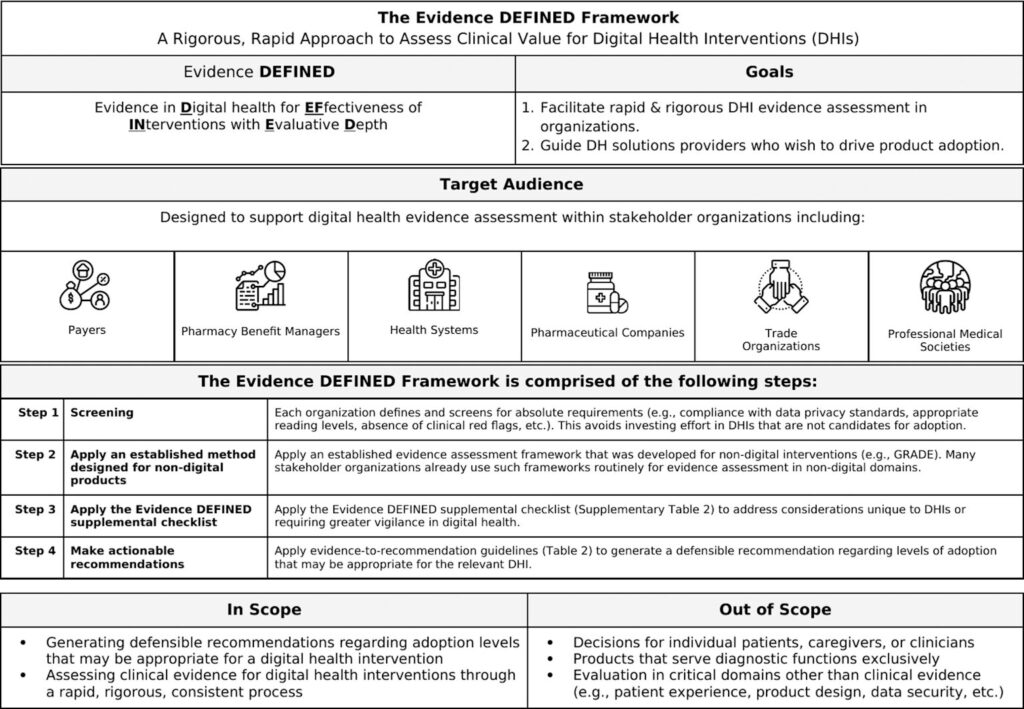
The Evidence DEFINED Framework outlines a rigorous, stepwise approach to assess the clinical value of digital health interventions, supporting organizations in making evidence-based adoption decisions
Cardiovascular Risk Assessment Tools
Cardiovascular disease remains the leading cause of mortality worldwide, making accurate risk prediction essential for effective preventive care and clinical decision-making. The evolution of cardiovascular risk calculators reflects advancing medical knowledge, improved data quality, and the integration of novel risk factors that enhance prediction accuracy.
American Heart Association PREVENT Calculator
The PREVENT (Predicting Risk of Cardiovascular Disease EVENTs) calculator represents the most significant advancement in cardiovascular risk assessment in over a decade. Developed using data from over 6.5 million U.S. adults, PREVENT provides both 10-year and 30-year risk estimates for total cardiovascular disease, atherosclerotic cardiovascular disease, and heart failure. The calculator’s revolutionary approach incorporates cardiovascular, kidney, and metabolic health measures while excluding race as a risk factor, recognizing it as a social rather than biological construct.
PREVENT’s superior performance compared to previous calculators has been demonstrated through extensive validation studies showing excellent discrimination with a C-statistic of 0.89 and significant improvement in risk reclassification. The tool’s integration of optional predictors including urine albumin-creatinine ratio, hemoglobin A1c, and social deprivation index enables more personalized risk assessment. The 2025 AHA/ACC High Blood Pressure Guideline has already incorporated PREVENT recommendations, establishing a 10-year total CVD risk threshold of ≥7.5% for initiating antihypertensive therapy in Stage 1 hypertension.
ASCVD Risk Estimator Plus
The American College of Cardiology and American Heart Association’s ASCVD Risk Estimator Plus remains widely adopted in clinical practice despite being superseded by PREVENT. The calculator estimates 10-year risk of atherosclerotic cardiovascular disease for adults ages 40-79 and provides lifetime risk estimates for younger individuals. Its strength lies in therapy impact assessment, allowing clinicians to demonstrate how specific interventions such as statin therapy or blood pressure management can reduce calculated risk.
The ASCVD calculator’s integration with electronic health records and clinical decision support systems has facilitated widespread adoption. However, validation studies have revealed significant limitations, particularly overestimation of risk in diverse populations and suboptimal calibration across different healthcare systems. These limitations underscore the importance of transitioning to more contemporary tools like PREVENT while maintaining awareness of the calculator’s specific strengths in therapy impact visualization.
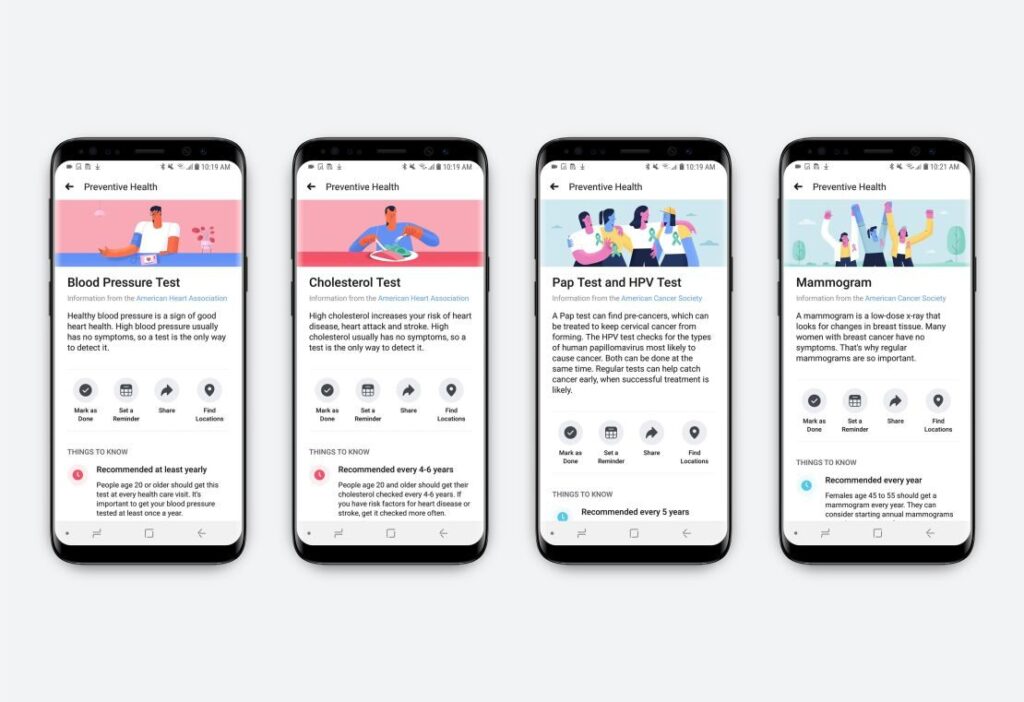
Preventive health app showing interactive screening tools for blood pressure, cholesterol, pap test, and mammogram with information and reminders
Framingham Risk Score Evolution
The Framingham Risk Score represents the foundation of modern cardiovascular risk prediction, with multiple iterations reflecting evolving medical knowledge. The original coronary heart disease risk score has been supplemented by comprehensive cardiovascular disease risk models that include stroke, heart failure, and peripheral arterial disease. Despite its historical importance, comparative studies suggest that updated tools like PREVENT offer superior discrimination and calibration in contemporary populations.
The continued relevance of Framingham-based tools lies in their extensive validation across diverse populations and integration with established clinical guidelines. However, healthcare providers must recognize that Framingham-derived risk estimates may underestimate or overestimate risk depending on population characteristics and contemporary risk factor prevalence. The tool’s simplicity and widespread familiarity ensure its ongoing utility in clinical settings where more sophisticated calculators are unavailable.
MESA Risk Score and Coronary Calcium Integration
The Multi-Ethnic Study of Atherosclerosis (MESA) Risk Score represents an important advancement in incorporating coronary artery calcium (CAC) scoring into risk assessment. The calculator provides 10-year coronary heart disease risk estimates both with and without CAC information, enabling clinicians to quantify the added value of coronary calcium testing. The innovative “coronary age” concept translates complex risk calculations into easily understood terms by expressing an individual’s risk as equivalent to that of an average person of a different age.
MESA’s validation across multiple ethnic groups and integration with mobile applications enhance its practical utility. The tool’s ability to demonstrate risk both before and after CAC testing supports informed decision-making about advanced cardiac imaging. While MESA focuses specifically on coronary heart disease rather than comprehensive cardiovascular risk, its precision in CAC integration makes it valuable for selected clinical scenarios requiring detailed cardiac risk assessment.
Cancer Risk Assessment and Screening Tools
Cancer prevention through risk assessment and early detection represents one of the most successful applications of interactive health assessment tools. These sophisticated calculators integrate genetic, environmental, and lifestyle factors to provide personalized cancer risk estimates and screening recommendations.
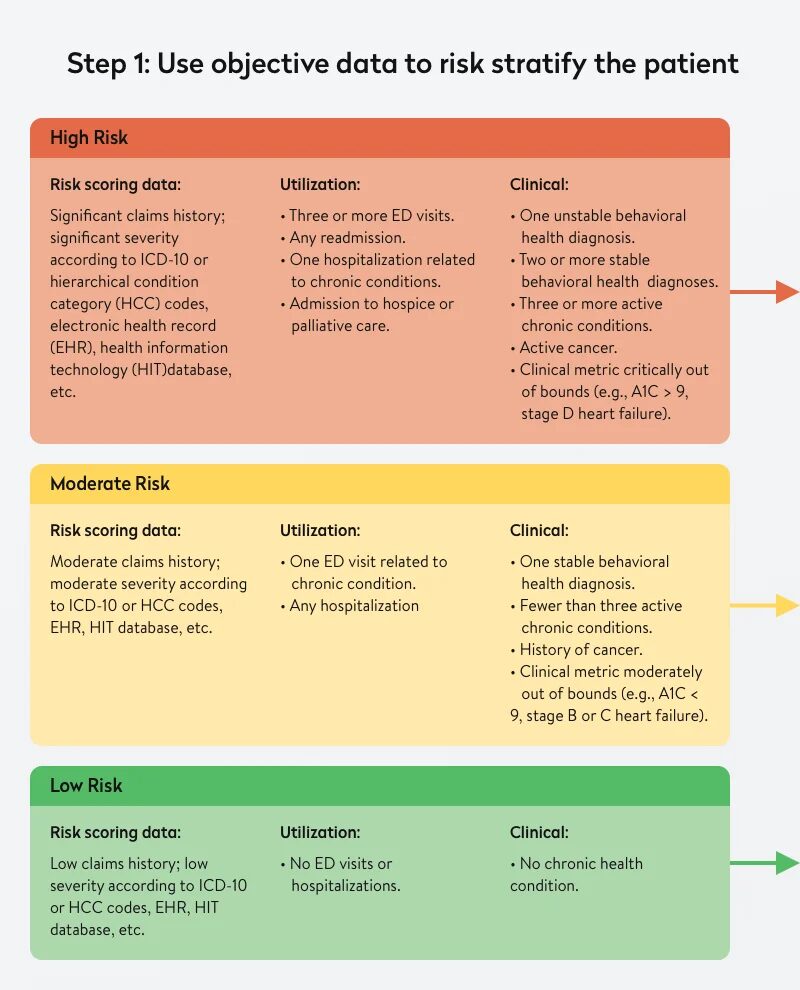
Using objective data to classify patients into high, moderate, and low risk categories based on clinical, utilization, and claims data
Comprehensive Multi-Cancer Assessment Tools
The Your Disease Risk Assessment Tool, developed by Washington University School of Medicine, provides risk assessments for 12 different cancers plus four major chronic diseases including heart disease, stroke, diabetes, and osteoporosis. This comprehensive approach recognizes the interconnected nature of chronic disease risk factors and promotes holistic lifestyle modifications for disease prevention. The tool’s 20-year track record includes published validation studies demonstrating well-calibrated risk estimates with discriminatory accuracy exceeding many other cancer risk prediction tools.
The American Cancer Society’s CancerRisk360 represents the newest generation of comprehensive cancer risk assessment. This tool evaluates family health history, personal health history, daily habits and lifestyle, and cancer screening history to provide personalized risk reduction recommendations. Unlike tools that provide numeric risk scores, CancerRisk360 focuses on actionable steps individuals can take to reduce cancer risk, recognizing that numeric risk estimates may not effectively motivate behavior change.
Breast and Ovarian Cancer Risk Assessment
The Breast Cancer Risk Assessment Tool (BCRAT), commonly known as the Gail Model, represents the gold standard for breast cancer risk prediction. Developed by the National Cancer Institute, BCRAT estimates 5-year and lifetime risk of developing invasive breast cancer using personal medical and reproductive history along with family history of breast cancer among first-degree relatives. The tool has been validated for white, Black/African American, Hispanic, and Asian/Pacific Islander women, though accuracy limitations exist for certain subgroups.
CanRisk represents the most sophisticated breast and ovarian cancer risk assessment tool available to healthcare professionals. This tool integrates BRCA1 and BRCA2 genetic testing results, polygenic risk scores, mammographic density, and comprehensive family history to provide highly personalized risk estimates. CanRisk’s endorsement by major medical organizations including NICE, NCCN, and ESMO demonstrates its clinical utility for genetic counseling and high-risk patient management.
Colorectal Cancer Risk Assessment
The National Cancer Institute’s Colorectal Cancer Risk Assessment Tool (CCRAT) provides 5-year and lifetime risk estimates for colorectal cancer among adults aged 45-85. The tool incorporates age, gender, race/ethnicity, family history, personal medical history, and lifestyle factors to generate personalized risk estimates. CCRAT’s validation across multiple ethnic groups addresses the growing recognition that cancer risk assessment tools must account for population diversity.
The tool’s integration with colorectal cancer screening guidelines enhances its clinical utility by connecting risk assessment with appropriate screening recommendations. However, CCRAT cannot accurately estimate risk for individuals with inflammatory bowel disease, inherited cancer syndromes, or personal history of colorectal cancer, highlighting the need for specialized assessment approaches for high-risk populations.
Mental Health Screening and Assessment Tools
Mental health screening represents a critical application of interactive assessment tools, enabling early identification and intervention for psychiatric conditions. The integration of validated screening instruments into digital platforms has dramatically improved access to mental health assessment while maintaining clinical rigor.

A person completing a digital health assessment form on a tablet, demonstrating interactive health screening tools
Depression and Anxiety Screening Instruments
The Patient Health Questionnaire-9 (PHQ-9) has become the most widely used depression screening tool in clinical practice. This multipurpose instrument screens for depression, monitors symptom severity, and tracks treatment response over time. The PHQ-9’s established cutpoints for mild (5), moderate (10), moderately severe (15), and severe (20) depression enable standardized assessment across diverse clinical settings. Importantly, question 9 serves as a critical suicide risk screening question that triggers additional assessment protocols.
The Generalized Anxiety Disorder-7 (GAD-7) questionnaire provides parallel functionality for anxiety assessment. This brief, validated instrument enables rapid screening for generalized anxiety disorder while also detecting panic disorder, social anxiety disorder, and post-traumatic stress disorder. The GAD-7’s brevity (7 questions) and established clinical cutpoints make it ideal for integration into routine clinical workflows and patient-facing digital platforms.
Comprehensive Mental Health Screening Platforms
Mental Health America’s screening platform and similar comprehensive tools provide access to validated screening instruments for multiple psychiatric conditions. These platforms typically include screens for depression, anxiety, bipolar disorder, post-traumatic stress disorder, eating disorders, substance use disorders, and psychosis. The anonymous, self-administered format removes barriers to mental health assessment while providing immediate feedback and referral resources.
The Columbia Suicide Severity Rating Scale (C-SSRS) represents the gold standard for suicide risk assessment across age groups from 5 years to adulthood. Available in 103 languages, the C-SSRS requires completion of a 30-minute online training program for certification. This comprehensive approach ensures that suicide risk assessment maintains clinical rigor while enabling widespread implementation across diverse healthcare settings.
Adolescent and Substance Use Screening
The CRAFFT screening questionnaire addresses the critical need for adolescent substance abuse assessment. This validated tool screens for high-risk alcohol and drug use disorders among individuals up to age 20, with the acronym derived from key words in each screening question. The American Academy of Pediatrics endorses CRAFFT for routine adolescent care, reflecting its clinical utility and validation in pediatric populations.
Specialized screening tools for specific substance use patterns, including the e-CHUG (alcohol) and e-TOKE (marijuana) assessments, provide detailed feedback about substance use patterns and associated risks. These tools enable anonymous self-assessment with personalized feedback, supporting harm reduction approaches and motivating behavior change through personalized risk communication.
Diabetes and Metabolic Risk Assessment
Diabetes prevention represents one of the most successful applications of population-based risk screening and intervention. Interactive diabetes risk assessment tools have enabled identification of high-risk individuals for targeted prevention programs, contributing to measurable reductions in diabetes incidence rates.
Prediabetes and Type 2 Diabetes Risk Assessment
The CDC Prediabetes Risk Test, developed collaboratively with the American Diabetes Association, provides rapid assessment of type 2 diabetes and prediabetes risk. This validated screening tool considers age, gender, gestational diabetes history, family history, hypertension, physical activity, and weight category to generate risk scores. Individuals scoring 5 or higher are identified as having increased risk for prediabetes and high risk for type 2 diabetes, warranting clinical evaluation.
The International Diabetes Federation’s Test2Prevent tool, based on the Finnish Diabetes Risk Score (FINDRISC), provides 10-year diabetes risk assessment with emphasis on modifiable risk factors. This tool’s strength lies in its focus on lifestyle factors that individuals can modify, including weight management, physical activity, and dietary habits. The assessment’s integration with diabetes prevention program referrals creates a seamless pathway from risk identification to intervention.
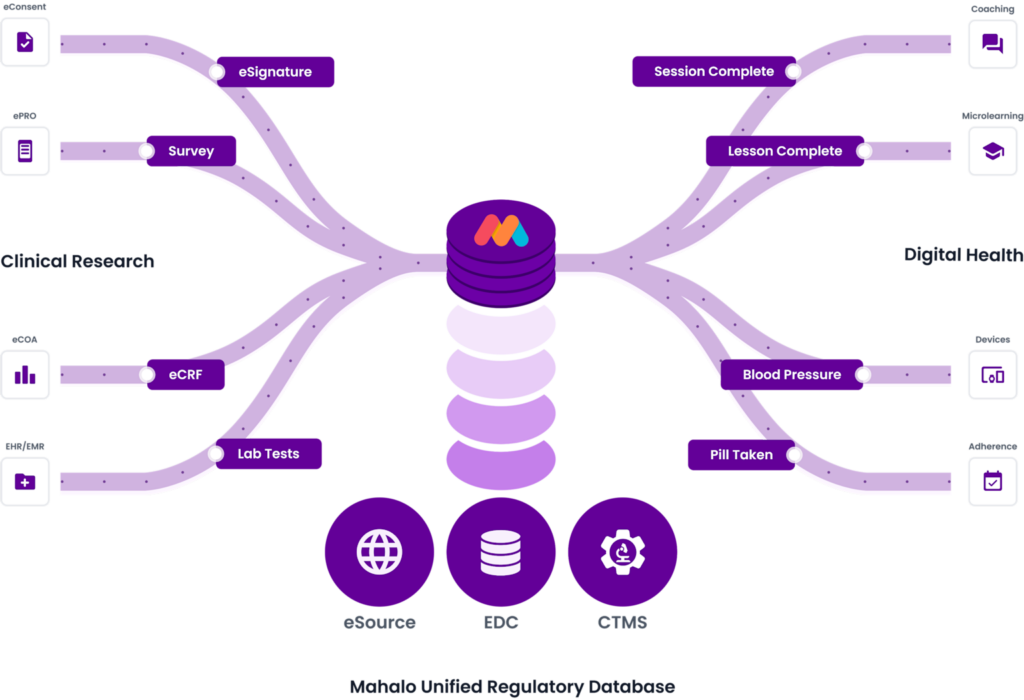
Integration of clinical research and digital health data into a unified regulatory database for comprehensive health assessment
Specialized Diabetes Risk Tools
Diabetes UK’s Know Your Risk tool represents a sophisticated approach to diabetes risk assessment that incorporates ethnicity-specific risk factors and waist circumference measurements. The tool recognizes that diabetes risk varies significantly across ethnic groups and adjusts risk calculations accordingly. The platform’s integration with follow-up support programs, including personalized email series and telephone consultations, demonstrates comprehensive approaches to diabetes prevention.
The American Diabetes Association’s risk assessment platform includes multiple complementary tools for diabetes education and self-management. These tools encompass A1C education, BMI calculation, and lifestyle modification guidance, creating a comprehensive resource for diabetes prevention and management. The platform’s emphasis on connecting users with healthcare providers ensures that risk assessment leads to appropriate clinical follow-up.
Surgical Risk Assessment and Operative Planning
Surgical risk assessment tools have revolutionized perioperative care by providing objective, data-driven risk stratification that enhances surgical decision-making and patient counseling. These sophisticated calculators integrate patient-specific factors with large surgical databases to generate accurate predictions of operative complications and mortality.
General Surgery Risk Assessment
The American College of Surgeons National Surgical Quality Improvement Program (ACS NSQIP) Surgical Risk Calculator represents the gold standard for general surgical risk assessment. This tool uses preoperative patient information to estimate risks of death and specific complications including surgical site infections, pneumonia, cardiac complications, and venous thromboembolism. The calculator’s database includes millions of surgical cases, ensuring statistical robustness and clinical relevance across diverse surgical procedures.
The NSQIP calculator’s strength lies in its procedure-specific risk estimation and continuous database updates that occur every three months. This dynamic approach ensures that risk calculations reflect contemporary surgical outcomes and evolving practices. The tool’s integration capabilities with electronic health records facilitate seamless incorporation into clinical workflows. However, the calculator’s disclaimer emphasizes that risk estimates are ballpark approximations that must be interpreted within the context of individual patient factors not captured by the algorithm.
Cardiac Surgery Risk Assessment
The Society of Thoracic Surgeons Adult Cardiac Surgery Database (STS ACSD) Operative Risk Calculator provides specialized risk assessment for cardiac surgical procedures. This tool estimates risks of operative mortality, major morbidity, and short-term outcomes for the vast majority of adult cardiac surgeries. The calculator’s mobile-friendly interface and simplified user design enhance its utility for patient-physician decision-making.
The STS calculator’s real-time risk estimation updates automatically with each user input, providing immediate feedback on how specific patient factors influence surgical risk. Clinical summaries generated by the tool can be easily copied into electronic health records, facilitating documentation and communication. The calculator’s coverage of more than 90 percent of adult heart surgeries performed nationally ensures broad applicability across cardiac surgery programs.
Clinical Decision Support Integration and Validation
The effectiveness of interactive risk calculators depends critically on their integration into clinical workflows and validation in real-world healthcare settings. Understanding the principles of clinical decision support systems and evidence-based tool evaluation enables healthcare organizations to select and implement the most appropriate assessment tools for their patient populations.
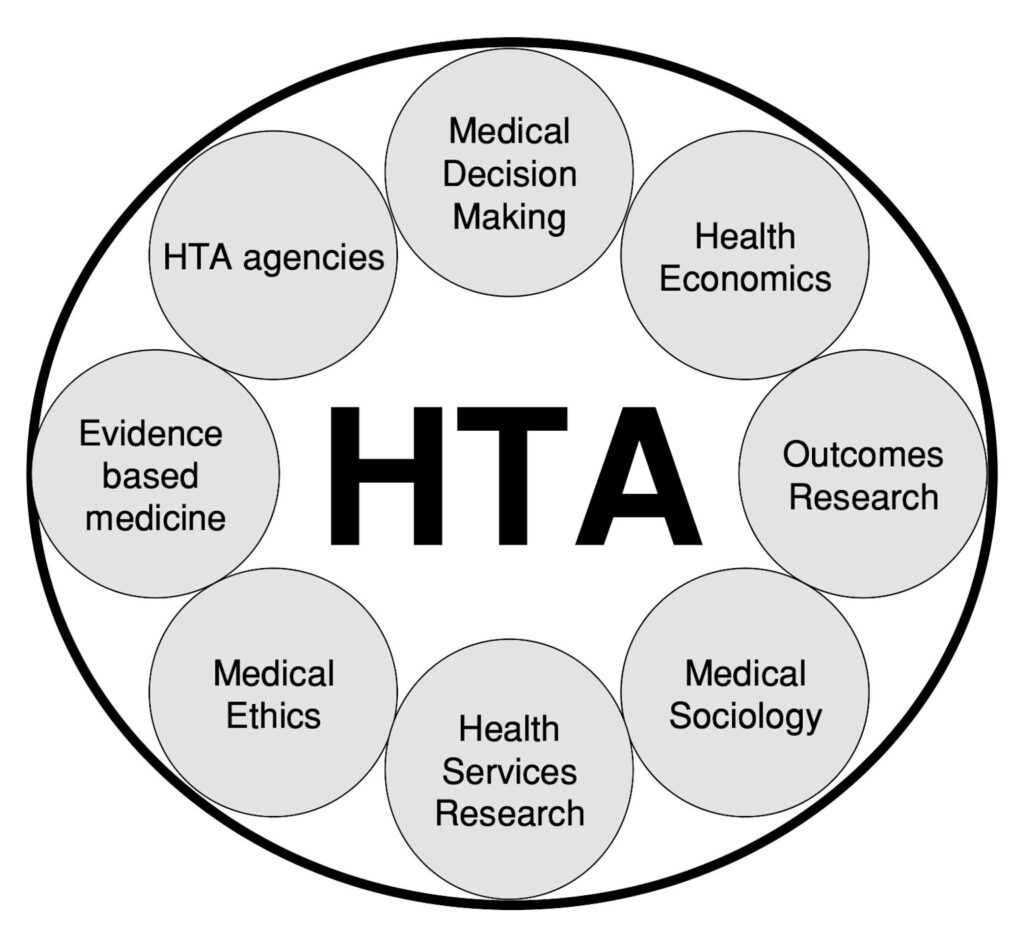
Health Technology Assessment (HTA) encompasses multiple disciplines including medical decision making, health economics, outcomes research, medical sociology, health services research, medical ethics, evidence-based medicine, and is supported by HTA agencies
Clinical Decision Support System Framework
Clinical Decision Support (CDS) systems encompass a broad range of tools designed to enhance clinical decision-making through the provision of patient-specific information and evidence-based recommendations. Interactive risk calculators represent a specific category of CDS tools that focus on risk stratification and preventive care guidance. The most effective CDS implementations integrate seamlessly with electronic health records, provide real-time decision support, and maintain user-friendly interfaces that minimize cognitive burden.
The architecture of modern CDS systems enables integration of risk calculators with other clinical tools including alerts and reminders, clinical practice guidelines, diagnostic support systems, and patient education resources. This comprehensive approach ensures that risk assessment leads to appropriate clinical actions and patient engagement. Organizations implementing CDS tools must consider factors including workflow integration, user training, and ongoing maintenance to ensure sustained utilization and clinical impact.
Validation and Accuracy Considerations
The accuracy of risk assessment tools varies significantly based on the populations in which they are applied and the healthcare systems implementing them. External validation studies consistently demonstrate that risk calculators perform differently across diverse patient populations, healthcare settings, and geographic regions. This variability underscores the importance of selecting tools that have been validated in populations similar to those being assessed.
Comparative studies of cardiovascular risk calculators reveal substantial disagreement between tools, with one in three paired comparisons disagreeing on risk category assignment. This disagreement stems from differences in derivation databases, clinical endpoints, risk interval duration, and population characteristics. Healthcare providers must understand these limitations and interpret risk calculator results as “ballpark approximations” that require clinical judgment for appropriate application.
Recent validation studies of the PREVENT calculator demonstrate both strengths and limitations in real-world implementation. While PREVENT shows excellent discrimination in some healthcare systems, it exhibits variable calibration across different patient populations and healthcare settings. The calculator tends to underestimate risk in certain populations, particularly those with specific comorbidities or demographic characteristics. These findings highlight the need for ongoing validation and potential calibration adjustments as tools are implemented across diverse healthcare environments.
Technology Integration and User Experience Design
The clinical impact of interactive risk calculators depends as much on user experience design and technology integration as on statistical accuracy and clinical validation. Modern assessment tools must balance comprehensive risk evaluation with user-friendly interfaces that encourage completion and clinical utilization.
Digital health interface showcasing self-regulation tools and activity tracking across tablet, smartwatch, and smartphone devices
Digital Platform Design Principles
Effective risk assessment tools prioritize intuitive user interfaces that minimize completion time while maintaining clinical rigor. The most successful platforms incorporate automated calculations that update in real-time as users input data, providing immediate feedback and enhancing engagement. Mobile-responsive design ensures accessibility across devices, recognizing that both healthcare providers and patients increasingly access tools through smartphones and tablets.
User experience research demonstrates that successful health assessment tools provide clear instructions, handle missing data gracefully, and offer contextual help for complex questions. The integration of visual elements, including progress indicators, risk visualizations, and personalized reports, enhances user comprehension and completion rates. Tools that provide printable results enable sharing with healthcare providers, creating continuity between self-assessment and clinical care.
Integration with Electronic Health Records
The seamless integration of risk calculators with electronic health record systems represents a critical factor in clinical adoption and impact. Tools that can be embedded within clinical workflows, automatically populate with patient data, and generate results that can be easily documented in medical records demonstrate superior utilization rates. Some healthcare systems have successfully integrated tools like PREVENT directly into their electronic health records, enabling real-time risk assessment during patient encounters.
Advanced integration approaches include the development of clinical decision support alerts that prompt risk assessment at appropriate clinical intervals, automated risk stratification for population health management, and integration with patient portals to enable patient-facing assessment tools. These sophisticated implementations require careful attention to workflow design, user training, and ongoing technical support.
Emerging Innovations and Future Directions
The future of interactive risk assessment tools lies in the integration of artificial intelligence, personalized medicine approaches, and population health management strategies. Emerging technologies promise to enhance accuracy, personalization, and clinical utility while addressing current limitations in risk prediction and patient engagement.

People collaboratively analyzing health technology data and assessments to evaluate healthcare tools
Artificial Intelligence and Machine Learning Integration
Advanced machine learning techniques offer the potential to improve risk prediction accuracy by identifying complex patterns in large datasets that traditional statistical models may miss. These approaches can incorporate non-traditional data sources including social determinants of health, environmental factors, and behavioral patterns derived from digital health platforms. The integration of artificial intelligence with existing risk calculators could enable continuous model refinement based on real-world outcomes data.
However, the implementation of AI-enhanced risk assessment tools requires careful attention to bias mitigation, interpretability, and regulatory compliance. Healthcare organizations must ensure that machine learning models remain transparent and clinically interpretable while addressing potential disparities in risk prediction across diverse populations. The development of explainable AI approaches for risk assessment represents an active area of research and development.
Personalized Medicine and Genomic Integration
The incorporation of genetic information into risk assessment tools represents a significant frontier for personalized prevention. Tools like CanRisk demonstrate the feasibility of integrating genetic test results, polygenic risk scores, and family history into comprehensive risk assessment. The Duke MeTree platform illustrates how genetic risk assessment can be combined with lifestyle factors and clinical data to provide holistic risk evaluation.
Future developments may include the integration of pharmacogenomics information to guide medication selection based on individual risk profiles, the incorporation of multi-omic data including metabolomics and proteomics, and the development of dynamic risk assessment tools that update continuously based on wearable device data and real-time health monitoring.
Population Health Management Integration
Risk assessment tools are increasingly being integrated into population health management strategies that identify high-risk individuals for targeted interventions. These approaches combine individual risk assessment with population-level analytics to optimize resource allocation and intervention targeting. Healthcare organizations are developing risk stratification protocols that use multiple assessment tools to create comprehensive risk profiles for their patient populations.
The integration of risk assessment tools with social determinants of health data, community resource mapping, and intervention tracking systems enables more comprehensive approaches to population health improvement. These sophisticated implementations require collaboration between clinical teams, population health specialists, and health information technology professionals.
Implementation Guidelines and Best Practices
Successful implementation of interactive risk calculators requires systematic approaches that address tool selection, workflow integration, user training, and ongoing quality improvement. Healthcare organizations benefit from structured implementation methodologies that ensure sustainable utilization and measurable clinical impact.
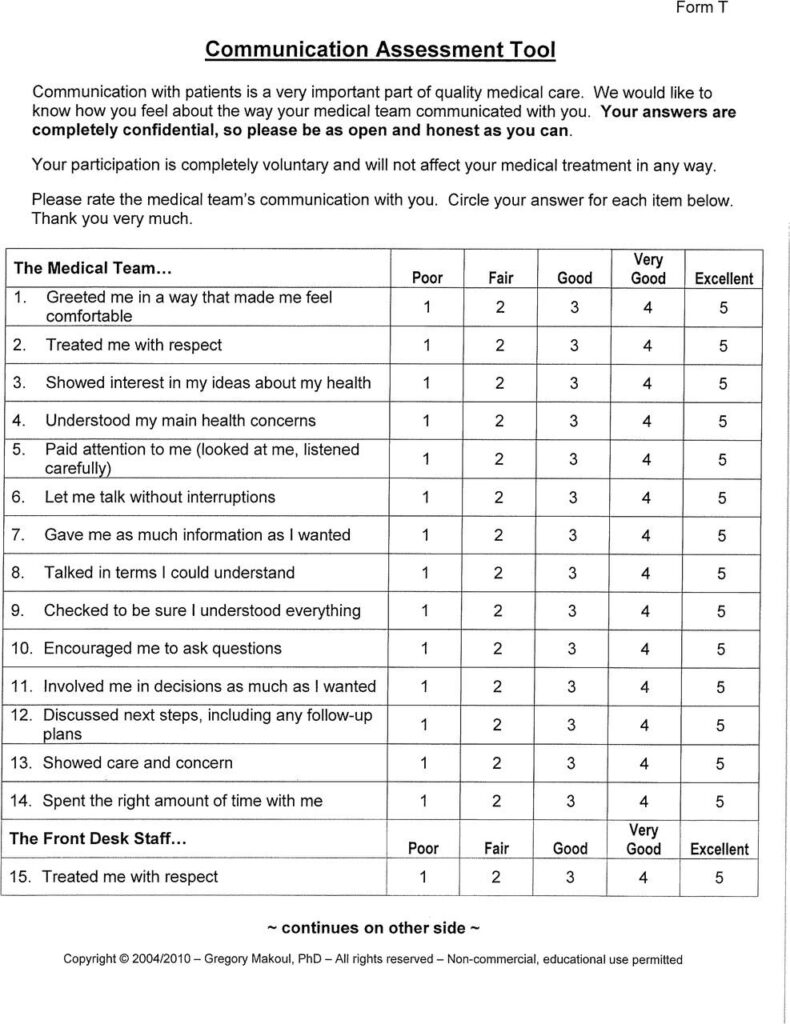
Patient communication assessment form for rating medical team and front desk staff on communication quality
Tool Selection and Evaluation Framework
Healthcare organizations should establish systematic criteria for evaluating and selecting risk assessment tools that align with their clinical priorities and patient populations. Key evaluation factors include validation in similar populations, integration capabilities with existing electronic health record systems, user interface design and usability, ongoing maintenance and update processes, and cost-effectiveness considerations. Organizations should prioritize tools that have demonstrated accuracy in external validation studies and provide transparent information about their development methodologies.
The evaluation process should include pilot testing with representative users, assessment of workflow integration requirements, and measurement of baseline clinical processes that the tools are intended to improve. Healthcare organizations should also consider the training requirements for successful implementation and the availability of ongoing technical support from tool developers.
Training and Change Management
Effective implementation requires comprehensive training programs that address both technical aspects of tool usage and clinical interpretation of results. Training should emphasize the limitations and appropriate clinical applications of risk assessment tools while providing practical guidance for patient counseling and shared decision-making. Healthcare organizations should develop competency-based training programs that ensure consistent tool utilization across clinical teams.
Change management strategies should address potential workflow disruptions, user resistance, and competing clinical priorities. Successful implementations often include clinical champions who advocate for tool adoption, feedback mechanisms that enable continuous improvement, and regular assessment of utilization rates and clinical outcomes. Organizations should also establish protocols for addressing technical issues and maintaining tool accuracy over time.
Quality Improvement and Outcomes Measurement
Healthcare organizations should establish metrics for evaluating the clinical impact and cost-effectiveness of risk assessment tool implementation. Key performance indicators may include tool utilization rates, accuracy of risk stratification, appropriate referrals for preventive interventions, patient satisfaction with risk communication, and measurable improvements in clinical outcomes. Regular assessment of these metrics enables continuous improvement and demonstrates the value of risk assessment tool investments.
Quality improvement initiatives should address identified gaps in tool accuracy, user satisfaction, and clinical outcomes. Organizations may need to calibrate tools for their specific patient populations, modify workflows to enhance utilization, or provide additional training to improve clinical interpretation. The most successful implementations maintain ongoing quality improvement processes that adapt to changing clinical needs and emerging evidence.
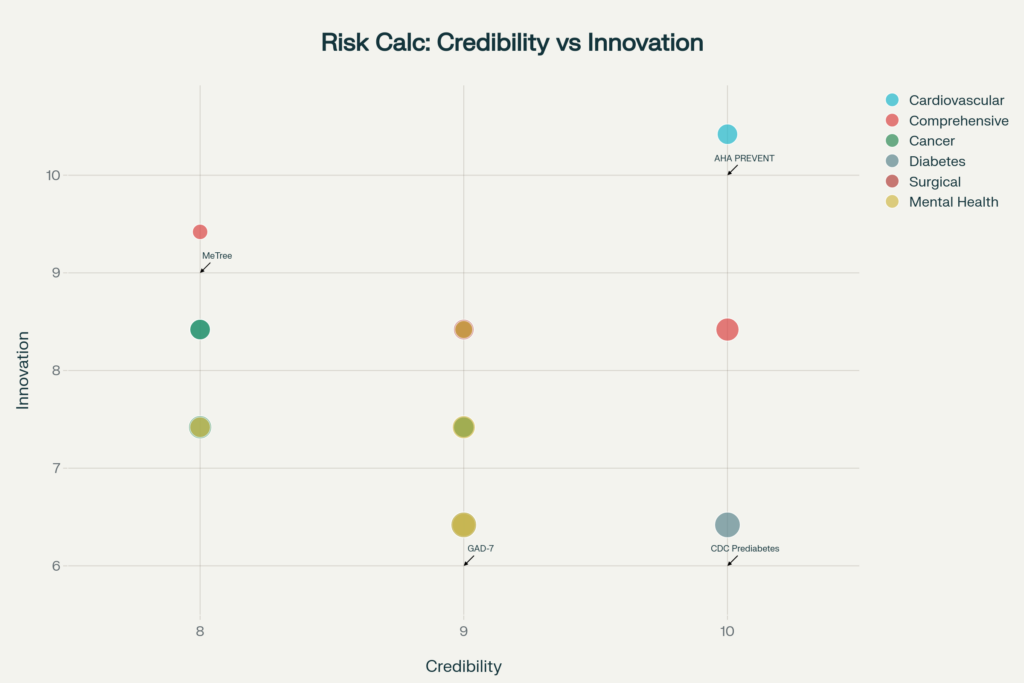
Interactive Risk Calculators Analysis: Credibility, Innovation, and Ease of Use comparison across different healthcare assessment categories
Conclusion
Interactive risk calculators and health assessment tools represent a fundamental transformation in preventive medicine, enabling personalized, evidence-based risk stratification that enhances clinical decision-making and patient engagement. This comprehensive analysis reveals that the highest-quality tools combine rigorous scientific validation with user-friendly design and seamless clinical integration. The American Heart Association’s PREVENT calculator exemplifies this balance, incorporating the most contemporary cardiovascular data while excluding problematic race-based adjustments and integrating novel risk factors including kidney and metabolic health measures.
The diversity of available assessment tools reflects the complexity of modern healthcare, with specialized calculators addressing cardiovascular risk, cancer screening, mental health assessment, diabetes prevention, and surgical planning. Each domain requires specific expertise and validation approaches, yet common principles emerge including the importance of population-specific validation, transparent methodology, and integration with clinical workflows. Tools that achieve widespread adoption typically demonstrate superior accuracy in external validation studies, provide actionable results that guide clinical decisions, and maintain user interfaces that encourage completion and clinical utilization.
The evidence demonstrates that no single risk calculator provides perfect accuracy across all populations and healthcare settings. This variability underscores the critical importance of healthcare providers understanding tool limitations, interpreting results within appropriate clinical contexts, and maintaining clinical judgment in risk assessment and management decisions. The most effective implementations combine multiple complementary tools with comprehensive clinical assessment and shared decision-making approaches that engage patients as partners in their preventive care.
Future developments in interactive risk assessment will likely emphasize artificial intelligence integration, personalized medicine approaches incorporating genetic and social determinants of health, and population health management applications. However, the fundamental principles identified in this analysis—rigorous validation, clinical utility, user-centered design, and continuous quality improvement—will remain essential for successful tool development and implementation. Healthcare organizations seeking to optimize their use of interactive risk assessment tools should prioritize systematic evaluation, comprehensive training, and ongoing quality improvement to ensure these powerful resources achieve their potential for improving preventive care and patient outcomes.
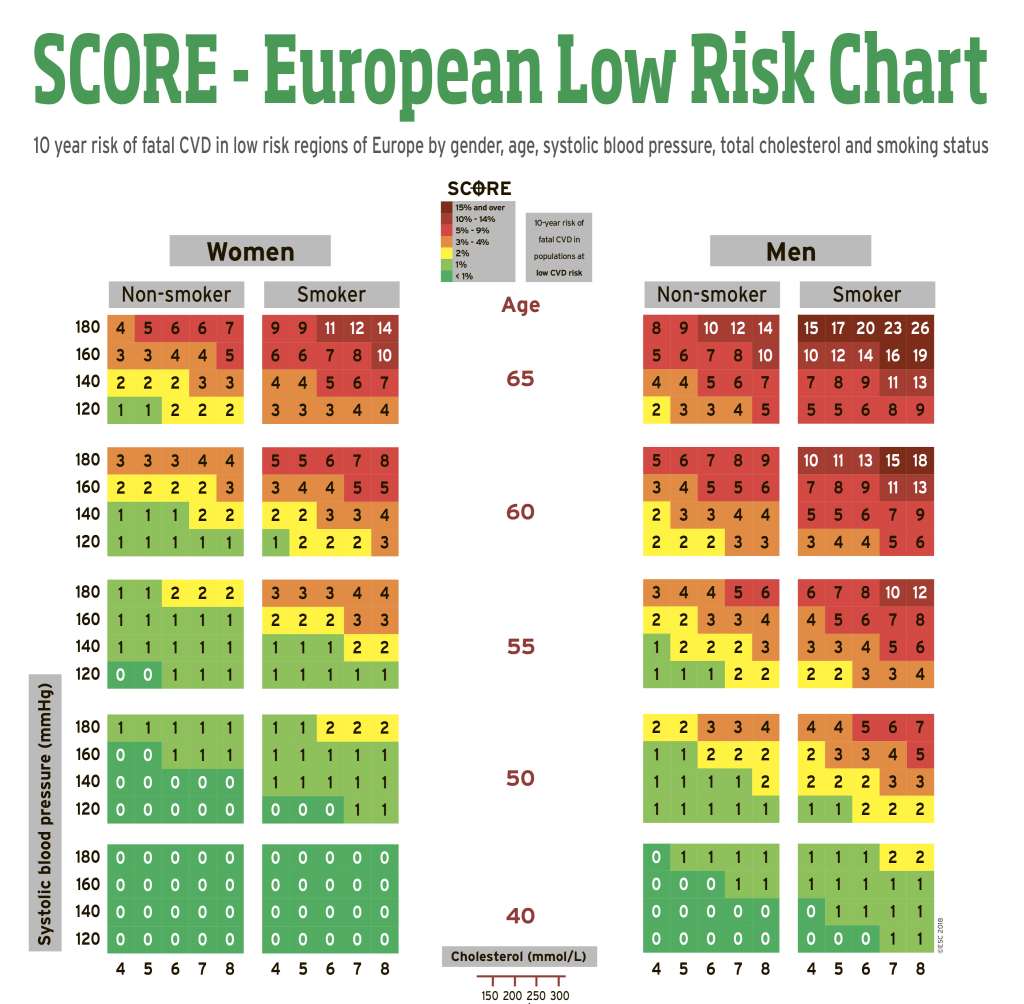
European cardiovascular risk chart showing 10-year fatal CVD risk by age, sex, smoking status, blood pressure, and cholesterol levels.